
My wife and I wore continuous glucose monitors and tested five of the worst foods for blood sugar levels. We then tried them again, this time with some common blood glucose “hacks” like apple cider vinegar and walking. Here’s how we got on:
The Worst Foods For Blood Glucose
My source was an article from Levels health, a company who specialise in continuous glucose monitoring. They used CGM data to pull out ten of the worst foods for blood glucose, from which I selected five:
- Breakfast cereal
- Instant Oatmeal
- Sushi
- Pizza
- Grapes
We then repeated each meal with something that is said to reduce the blood sugar spike. I should point out that even though we are non-diabetics, deliberately spiking your blood sugar is not healthy and we both felt the negative effects on energy levels, focus and hunger during this experiment.
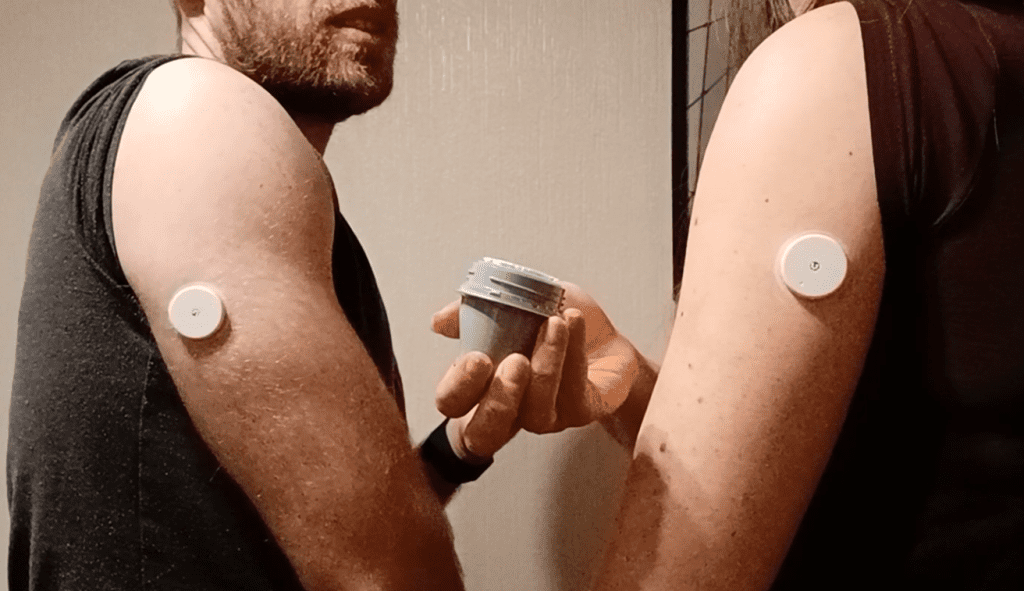
We measured the results in two ways:
- the peak value, so the highest our glucose reached in the two hours after a meal
- the AUC, the Area Under the Curve, which is a measure of the overall rise in blood sugar, and that’s calculated in the two hours after the first bite of food.
The order we ate the foods was randomised and it tended to be for breakfast or lunch. We remained seated for at least 90 minutes after the start of the meal to keep the experiment somewhat controlled. However, there were certainly factors beyond our understanding that may have influenced each result.
The Results
It makes sense to go through these one meal at a time. For a bit of context, it’s generally best to keep under 7.8 mmol/L, which is 140mg/dL in American units. Research has also shown that two people can have a completely different glucose response to exactly the same food. Graphs with the blue shading are my readings and the purple shading is my wife.
Breakfast Cereal
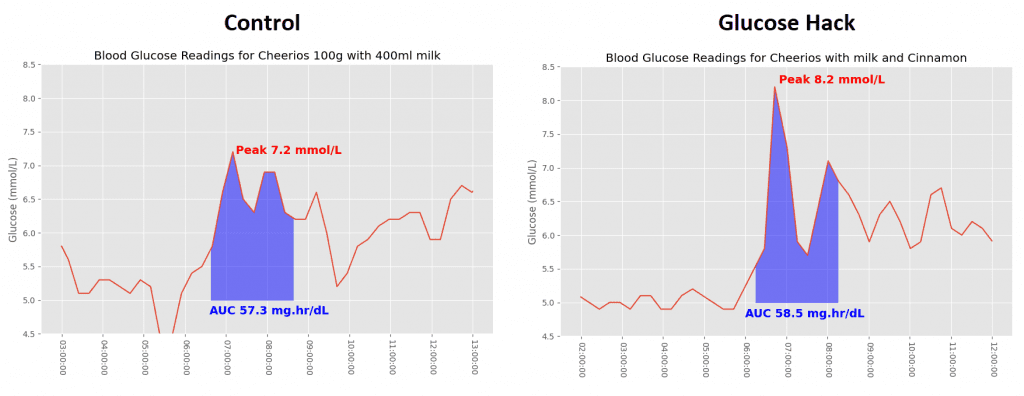
I aligned the portion size with what I would typically eat, around 100 grams, and my wife did the same, eating 80 grams. The second version of the meal included half a teaspoon of cinnamon, one of the glucose hacks. It has qualities that may reduce both fasting glucose and the post prandial (after eating) spike in both diabetics and non-diabetics.

Strangely, the serving with 1/2 teaspoon of cinnamon produced a higher glucose spike, though it came down faster. That meant a higher peak value and a very similar AUC of ~58 mg.hr/dL.
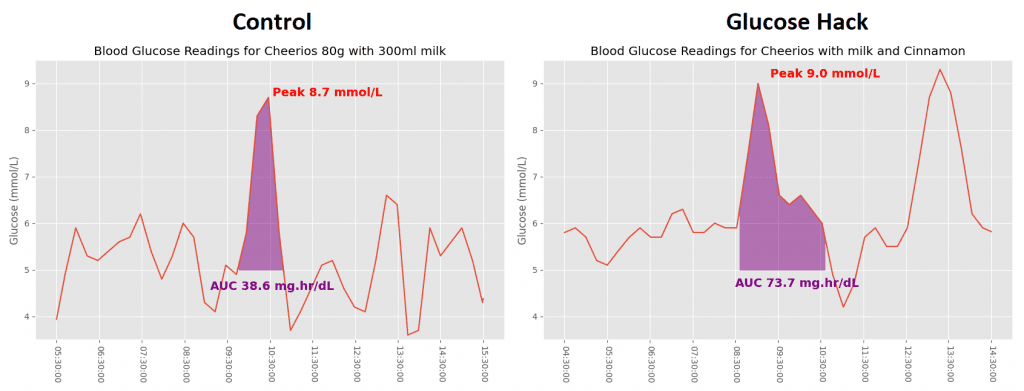
My wife had very similar peaks but her glucose levelled off sooner when cinnamon was added. For the plain cereal she had a very large drop from 8.7 mmol/L right down to 3.8 mmol/L, which can result in reactive hypoglycaemia.
Instant Oatmeal
I have a whole separate article on instant oatmeal and how terrible it is for blood glucose spikes. You can hopefully tell from the image below that the instant oatmeal is much finer than regular oatmeal. That means your body requires less effort to break it down into glucose molecules, and so it enters the bloodstream faster. That leads to a more pronounced glucose spike than you’d otherwise have with regular oatmeal.

There was an almost identical response from my blood sugar to the two meals. The only difference is the regular oatmeal peaked a touch higher and came down further before rebounding.
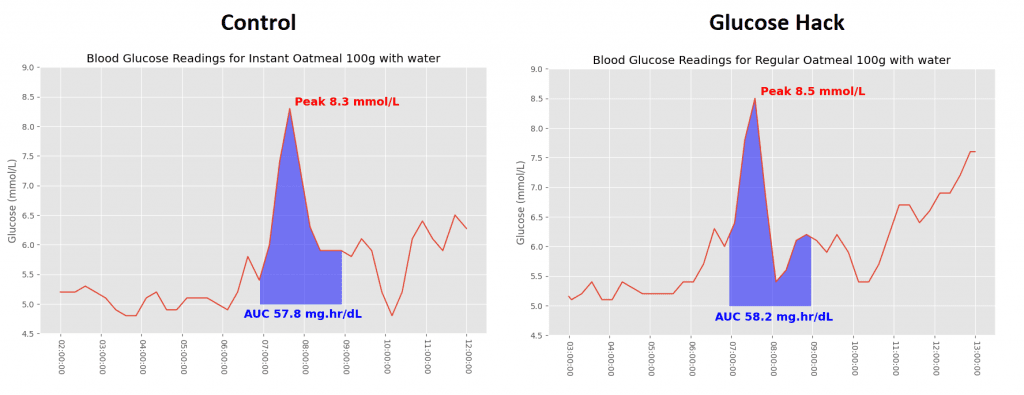
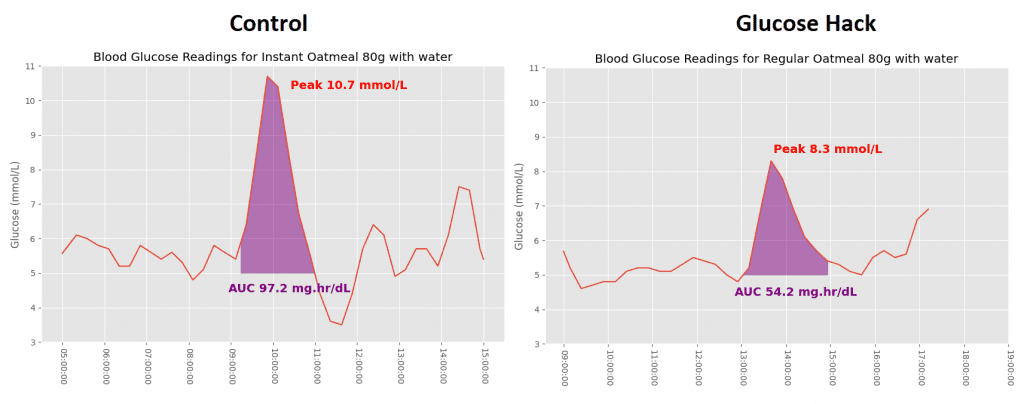
My wife had exactly the response you’d hope to see by switching from instant oatmeal to regular. The peak is far less pronounced, with instant oats giving her the highest peak of all meals at 10.7 mmol/L (192 mg/dL).
Sushi
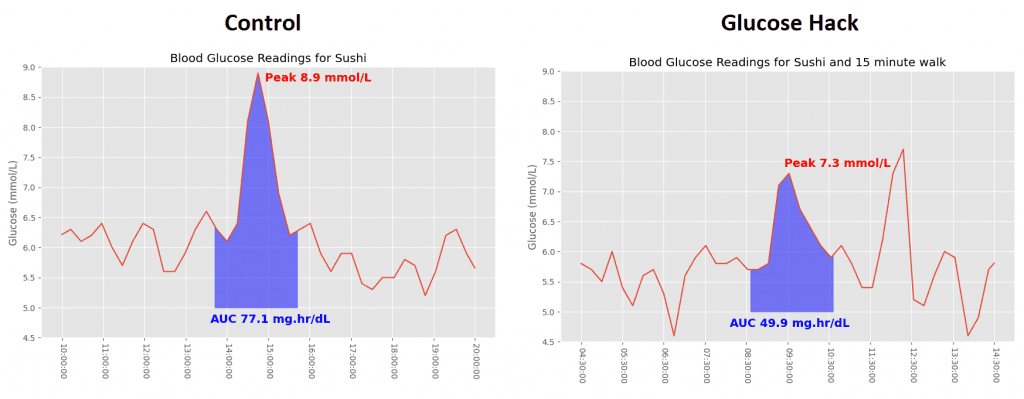
Sushi is a classic glucose spiker, with its white “sticky” rice being a key ingredient. We deliberately opted for Maki and Nigiri in order to maximise the rice content of the meal. Overall this packed 87 grams of carbohydrate and only 6 grams of fat (it was also delicious!). For the second meal we did 15 minutes of walking straight after the meal, which research shows can significantly reduce the glucose spike.

Most articles online agree that walking after a meal is the most effective way to blunt the glucose spike… and that’s exactly what I saw. There was a large reduction in the peak and the AUC was also far smaller. This was the most promising difference I saw across all five meal pairings.
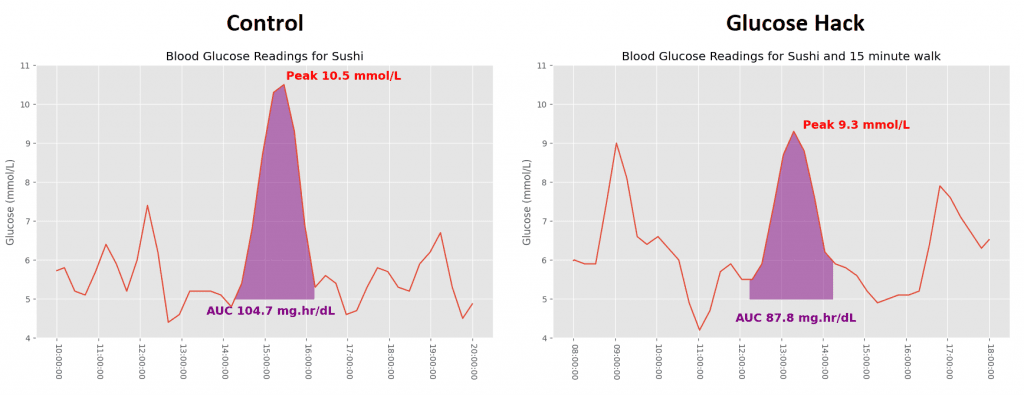
I was expecting an even bigger difference for my wife but the walking still resulted in quite a high peak glucose value. We chose to walk right after eating and then sit in a chair for the remainder of the two hours. Based on the research, maintaining some level of activity beyond the 15 minutes would have led to an even lower spike.
Pizza
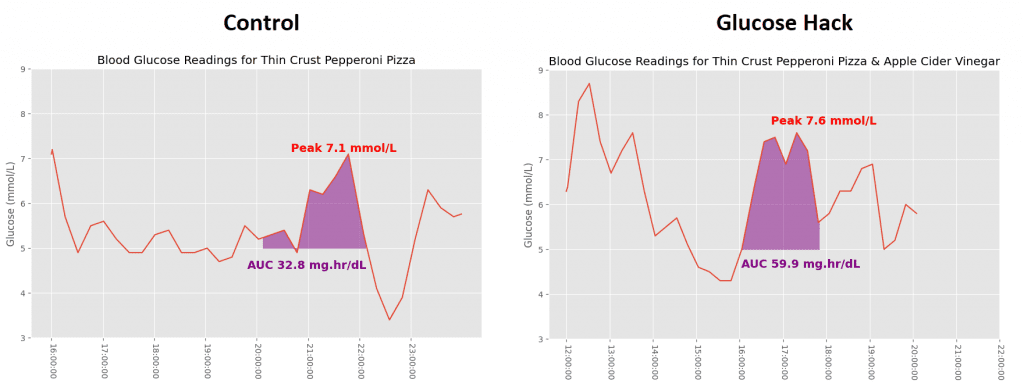
I found it unusual to see pizza on the list. It’s possible the CGM users who had high readings were choosing to eat deep dish pizza. I tend to eat thin crust pizza, making the carb to fat ratio more favourable for glucose response. This was paired with around 15ml of apple cider vinegar (ACV) in 45ml of water. The research on ACV is mixed, though improvements to HbA1c and fasting glucose have been seen.

My second graph here needs a quick explanation:
Across all these graphs, my decision was to calculate AUC from a baseline of 5.0 mmol/L, instead of the value I saw immediately before the meal. That’s because I thought peak values would be absolute rather than relative to the starting point. What that means is that I thought a meal was more likely to spike at e.g. 7.0 mmol/L whether my glucose is at 4.5 or 6 before the meal, as opposed to rising by a specific amount. I’ll be honest, I don’t know enough about the science to have strong opinions.
If you take into account where my glucose started for each meal, you could argue the Apple Cider Vinegar was effective. Unfortunately it was the hurry of trying to squeeze all these meals into a 14 day trial that meant I had to test a meal when my glucose was already above 6.5 mmol/L.
Oh, and if you’ve been paying attention to the x-axis, yes, I did eat pepperoni pizza for breakfast.
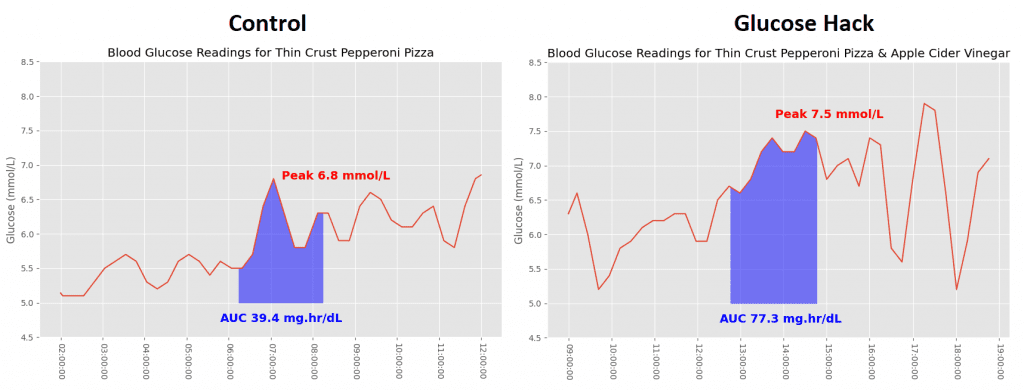
The inclusion of apple cider vinegar before the pizza meant a higher peak and higher AUC for my wife too. The pizza with apple cider vinegar test was done after a lunch which spiked her glucose to 8.7 mmol/L. It may be that a large glucose spike has a knock on effect on the subsequent meal, which would explain a lot. She was also in the luteal phase of her cycle which is known to produce some dramatic blood sugar rises due to the increase in progesterone.
Grapes
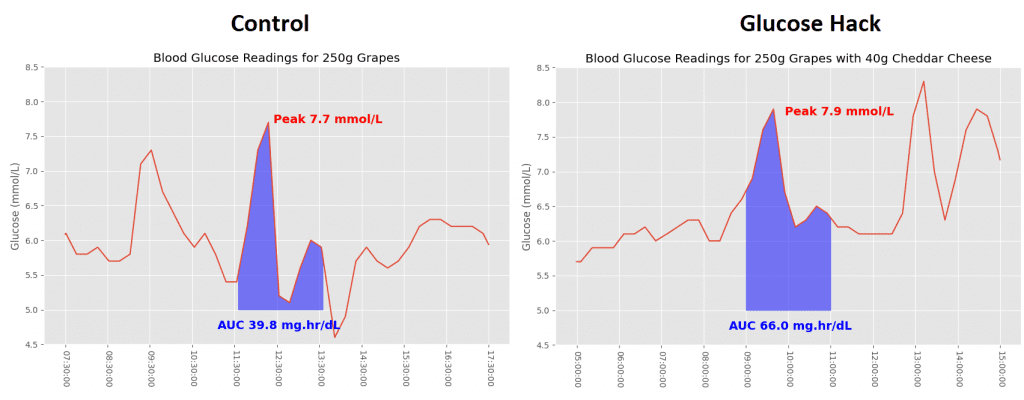
Grapes feature under the “surprising foods that spike your blood glucose”. Personally I’m not that surprised, I feel that macronutrient composition (protein, carbohydrate and fat) is a good measure of potential to spike glucose, and grapes are almost exclusively carbohydrate. Pictured below is the second meal, which has the addition of 40g cheddar cheese. The research shows that a ratio of 4 grams of fat for every 10 grams of carbohydrate reduces the overall glucose spike.

Once again you can see how my blood glucose levels either side of the meal has influenced the calculation of AUC. If you instead measure from the start of the meal then there’s a far more pronounced peak with grapes on their own.
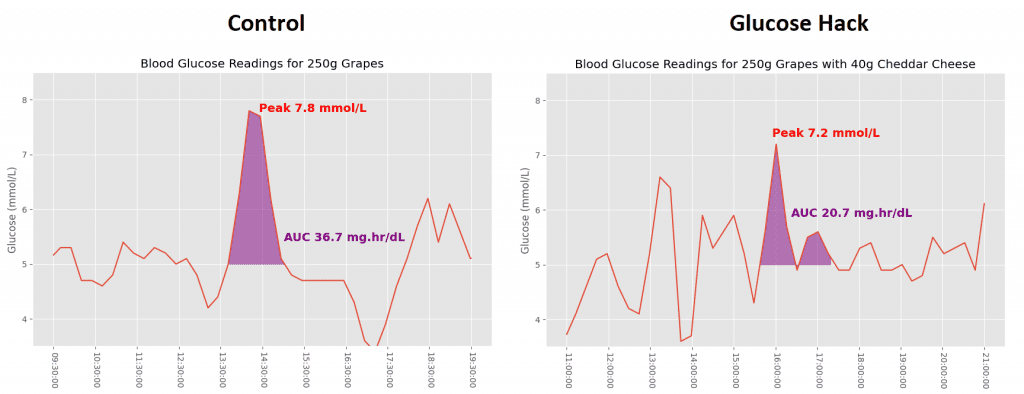
Grapes had a more reasonable effect for my wife, which is a good thing since she eats them almost every day! The cheese kept the spike down and gave her the lowest AUC of all meals. While it’s a positive for blood glucose, there are other health reasons which mean adding 40 grams of cheese to every meal isn’t a practical solution.
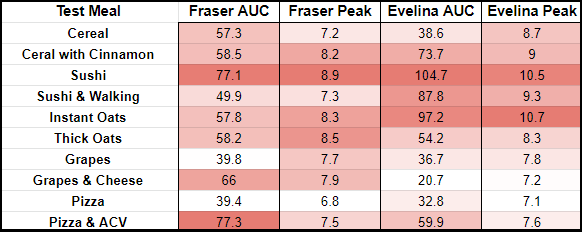
Summary
There wasn’t quite the dramatic improvement I was hoping for from the glucose “hacks” across the experiment as a whole. Factors we weren’t able to control could have impacted the results, causing the glucose hacks to look ineffective. The only meal we both saw a reduction in the glucose spike from was walking after a meal.
The latest glucose monitor apps might tell you to avoid foods that cause a dramatic spike. This experiment hopefully illustrates the need to test a food multiple times, as factors outside your control could make a “good” meal have a “bad” response (and vice versa). It’s also unlikely your meal is exactly the same each time, as even the order you eat it can have an effect.
Conclusion
Overall, adding cinnamon to a meal should be beneficial and it has other health properties outside of the effect on blood glucose. It’s sensible to avoid the extra processing that turns thick, steel cut oats into instant oats (all for the sake of 2 minutes cooking time) and that logic can be applied elsewhere. For example, another meal that causes glucose spikes is fruit smoothies, as blending breaks down the food before it’s eaten. For that reason it’s better to eat your fruit and vegetables in their original form.
Ultimately, the best advice is to introduce some low level activity after meals if you’re otherwise going to be sedentary. That doesn’t have to be brisk walking, something like housework or washing the dishes should also have a positive effect. While glucose response isn’t everything, there’s a whole host of benefits to maintaining stable levels, including energy levels, focus and how soon you feel hungry again.
Thanks for reading!

